Table of Contents
Vitamin B12 (cobalamin) is required for healthy nerve function and the synthesis of red blood cells and DNA. A deficiency in B12 increases inflammation and oxidative stress by raising homocysteine. High homocysteine, in turn, is associated with cardiovascular disease and decreased immune response. Vitamins B6, B9 (folate) and B12 break down homocysteine.1
B12 deficiency is also associated with many other physical, neurological and psychological symptoms, including migraines,2 certain respiratory disorders, depression and memory loss.3 Surprisingly, recent research4 suggests it may also be a key player in cellular regeneration.
B12 Required for Tissue Repair and Regeneration
As reported by Science Daily,5 “Vitamin B12 supplementation shows potential in speeding up tissue repair in a model of ulcerative colitis — an observation that points to potential new treatments for inflammatory diseases.”
More specifically, the study found that vitamin B12 is a limiting factor for tissue repair. In other words, to optimize tissue regeneration, you need sufficient amounts of B12 in your system. Science Daily explains:6
“The research was focused on an experimental process known as cellular reprogramming which is thought to mimic the early phases of tissue repair. The IRB team found that cellular reprogramming in mice consumes large amounts of vitamin B12.
Indeed, the depletion of vitamin B12 becomes a limiting factor that delays and impairs some aspects of the reprogramming process. Considering the abundance of vitamin B12 in the normal diet of mice, the investigators were surprised to observe that the simple supplementation of vitamin B12 significantly enhanced the efficiency of reprogramming.
The researchers validated their findings in a model of ulcerative colitis, demonstrating that the intestinal cells initiating repair undergo a process similar to cellular reprogramming and also benefit from vitamin B12 supplementation.”
B12 Is the Limiting Factor for Methylation
The reason B12 is so important in tissue regeneration has to do with its role in methylation. Methylation is one of several mechanisms cells use to control gene expression. When there’s damage to cells or tissues — whether due to injury, age, trauma or disease — reparative gene expression programs kick in to replace the damaged tissues.7
The DNA in the cells that need to be repaired require high levels of methylation, and B12, it turns out, is the limiting factor for methylation. Hence, you need high amounts of B12. If you don’t have enough, many genes end up not working properly, hence tissue regeneration is hampered as well. Co-lead author Marta Kovatcheva, Ph.D., explained it this way:8
“B12 is involved in just two metabolic reactions in mammals — including mice and humans — and one of these reactions is critical to [producing] a chemical tag, more technically [known as] ‘a methyl donor.’
This chemical group is used to ‘tag’ many regulatory proteins of the DNA and the DNA itself, and in doing so, the activity of the DNA is modified — the DNA is ‘reprogrammed.’ This ‘tagging’ is very complex and dynamic and, although not yet fully understood, it is key for determining the behavior of cells, including their ability to repair or regenerate tissue.
During critical periods, such as upon injury, cells require massive amounts of the ‘methyl tag’ and therefore B12 … so much so that despite a normal healthy diet, mice undergoing reprogramming suffer partial B12 deficiency. Supplementation with B12 facilitates reprogramming and tissue repair — it occurs faster and more widespread.
There are diseases that could also benefit, such as colon ulcers. In theory, every disease that involves an active process of injury could benefit from this.”
Research9 published in 2022 also found that vitamin B12, applied topically, can be helpful in the treatment of radiodermatitis, i.e., skin damaged by radiotherapy used in cancer treatment.
Vitamin B12 for Nonalcoholic Steatohepatitis
Another process in which B12 can be helpful is that of nonalcoholic steatohepatitis (NASH), for which there is no pharmaceutical treatment option. NASH is the second stage of nonalcoholic fatty liver disease (NAFLD). Even more advanced stages include fibrosis and cirrhosis, which significantly raises your risk of liver cancer.
In one 2022 study,10 supplementation with B12 and folic acid (B9) was shown to slow the progression of NASH and actually reverse fibrotic tissue changes in the liver. The researchers were seeking to understand the relationship between hyperhomocysteinemia (abnormally elevated homocysteine) and NASH.
Using an animal model, they administered vitamin B12 and folic acid, attempting to reverse the cellular features of NASH. What they discovered is that homocysteine attaches to and blocks a protein called syntaxin 17, thereby inducing NASH.
However, when mice were given supplemental vitamin B12 and folic acid, the levels of syntaxin 17 rose, which slowed the progression of NASH and reversed the fibrosis. One of the scientists in the study, Brijesh Singh, Ph.D., commented:11
“Our findings are both exciting and important because they suggest that a relatively inexpensive therapy, vitamin B12 and folic acid, could be used to prevent and/or delay the progression of NASH. Additionally, serum and hepatic homocysteine levels could serve as a biomarker for NASH severity.”
The researchers were excited by the possibilities since the early stages of NAFLD often have no symptoms, and if left undiagnosed and untreated, the condition can progress to NASH or fibrosis.
B Vitamins in COVID-19 Treatment
B vitamins are also important for healthy immune function, which is your first line of defense against all infections and diseases, both acute and chronic. An August 2020 paper, “Be Well: A Potential Role for Vitamin B in COVID-19,”12 made the case for B vitamin supplementation to minimize the risks associated with the infection.
B1, B2, B3, B5, B6, B9 and B12 can influence several COVID-19-specific disease processes, including viral replication and invasion, cytokine storm induction, adaptive immunity and hypercoagulability.13 In the graphic below, from the you can see which B vitamins are involved in each of these processes.
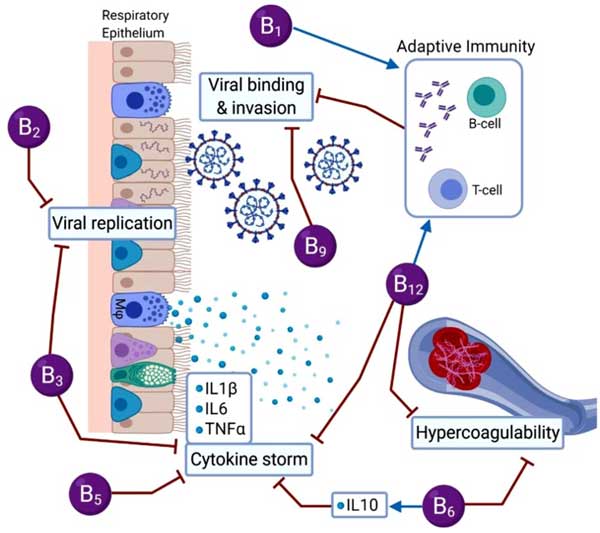
According to the authors, based on B vitamins’ effects on your immune system, immune-competence and red blood cells (which help fight infection), supplementation may be a useful adjunct to other COVID prevention and treatment strategies.14
“There is a need to highlight the importance of vitamin B because it plays a pivotal role in cell functioning, energy metabolism, and proper immune function,” they wrote.
“Vitamin B assists in proper activation of both the innate and adaptive immune responses, reduces pro-inflammatory cytokine levels, improves respiratory function, maintains endothelial integrity, prevents hypercoagulability and can reduce the length of stay in hospital.
Therefore, vitamin B status should be assessed in COVID-19 patients and vitamin B could be used as a non-pharmaceutical adjunct to current treatments …”
The paper goes on to detail how each B vitamin can be used to manage COVID-19 symptoms:
|
Vitamin B1 (thiamine) — Thiamine improves immune system function, protects cardiovascular health, inhibits inflammation and aids in healthy antibody responses. Vitamin B1 deficiency can result in an inadequate antibody response, thereby leading to more severe symptoms. There’s also evidence suggesting B1 may limit hypoxia. |
|
Vitamin B2 (riboflavin) — Riboflavin in combination with ultraviolet light has been shown to inhibit replication of the MERS-CoV virus. The combination has also been shown to decrease the infectious titer of SARS-CoV-2 below the detectable limit in human blood, plasma and platelet products. |
|
Vitamin B3 (niacin/nicotinamide) — Niacin is a building block of NAD+ and NADP, which are vital when combating inflammation. Nicotinamide also reduces viral replication and strengthens your body’s defense mechanisms, while niacin helps protect your lungs and strengthens immune function. |
|
Vitamin B5 (pantothenic acid) — Vitamin B5 aids in wound healing and reduces inflammation. |
|
Vitamin B6 (pyridoxal 5′-phosphate/pyridoxine) — Pyridoxal 5′-phosphate (PLP), the active form of vitamin B6, is a cofactor in several inflammatory pathways. Vitamin B6 deficiency is associated with dysregulated immune function. Inflammation increases the need for PLP, which can result in depletion. According to the authors, in COVID-19 patients with high levels of inflammation, B6 deficiency may be a contributing factor. What’s more, B6 may also play an important role in preventing the hypercoagulation seen in some COVID-19 patients. |
|
Vitamin B9 (folate/folic acid) — Folate, the natural form of B9 found in food, is required for the synthesis of DNA and protein in your adaptive immune response. Folic acid, the synthetic form typically found in supplements, was recently found15 to inhibit furin, an enzyme associated with viral infections, thereby preventing the SARS-CoV-2 spike protein from binding to and gaining entry into your cells. The research16 suggests folic acid may therefore be helpful during the early stages of COVID-19. Another recent paper17 found folic acid has a strong and stable binding affinity against SARS-CoV-2. This too suggests it may be a suitable therapeutic against COVID-19. |
|
Vitamin B12 (cobalamin) — As mentioned, B12 is required for the synthesis of red blood cells, and deficiency increases inflammation and oxidative stress. According to the authors:18
|
How to Improve Your Vitamin B Status
Advancing age can diminish your body’s ability to absorb B12 from food,19 so the need for supplementation increases as you get older. According to the National Institutes of Health,20 the rate of vitamin B12 deficiency in the U.S. is close to 20% in those older than 60.
Other data from a large, nationally representative sample21 demonstrated that serum levels of B12 are inversely associated with obesity, so those who are overweight or obese also need to be more mindful about their B12 intake.
Vitamin B12 is found almost exclusively in animal foods such as beef and beef liver, lamb, snapper, venison, salmon, shrimp, scallops, poultry, eggs and dairy products. The few plant foods that are sources of B12 are actually B12 analogs that block the uptake of true B12, so do not make the mistake of thinking you can rely on vegan sources for all your B12 needs.
If you rarely eat the foods listed, consider using nutritional yeast. It’s high in B12 and has a cheesy flavor that can work well on any number of dishes. It’s highly recommended for vegetarians and vegans. One 16-gram serving (just over 2 tablespoons22) provides 24 mcg of natural vitamin B12.23
Sublingual (under-the-tongue) fine mist spray or vitamin B12 injections are also effective, as they allow the large B12 molecule to be absorbed directly into your bloodstream. To ensure optimal absorption and utilization, opt for the methylated version, i.e., methylcobalamin, as it is far superior and more natural than the more common cyanocobalamin.




More Stories
Ashwagandha’s Impact on Cortisol Levels in Stressed People
Health care cyberattack ‘likely one of the worst,’ expert says
Accessing Medicinal Cannabis in the UK: A Comprehensive Guide